Changes in the Microbiological World
- sjpdragonlady
- Jan 27, 2024
- 13 min read
Multi-Drug Resistant Gonorrhea-- QuantuMD
What is antibiotic resistance?
Today we are taking a different perspective on our environment, and discussing the microscopic universe. Things that we do (such as taking antibiotics) impact germs such as fungi and bacteria, and alters the world around us, which affects our health. Antibiotic resistance is a public health problem that greatly harms many people. Antibiotic resistance develops in several ways. When people take antibiotics for infections, the antibiotics may kill some bacteria but be unable to kill other bacteria. The bacteria that has the ability to protect itself from those antibiotics will survive and reproduce themselves, leading to a higher percentage of resistant bacteria. These bacteria can infect other people, and may spread to the point that there are more resistant bacteria than bacteria which can be killed by antibiotics. Stronger and stronger antibiotics are required to treat infections caused by these bacteria. Some bacteria are extremely difficult to kill using existing antibiotics, and can cause chronic infections. As people take more antibiotics, bacteria becomes resistant to antibiotics more quickly, and infections are harder to treat. Similarly, widespread use of antibiotics to treat farm animals such as chickens, cows and pigs can lead to resistant food germs, which can also spread to people.
Antibiotic Resistance on Agar Plate, Shutterstock
How common is antibiotic resistance?
Center for Disease Control
According to the Center for Disease Control (CDC), each year in the United States there are more than 2.8 million antimicrobial-resistant infections (infections that will not get better with the usual antibiotic treatments). This equals one antimicrobial-resistant infection for every 119 people in the United States. These infections are directly responsible for at least 35,000 deaths annually. The cost of treating the 6 most common types of resistant infections is greater than $4.6 billion per year. Resistant infections are a particular health risk for patients who are hospitalized. The CDC estimates that almost 70% of infections caught by hospitalized patients are resistant to at least one of the antibiotics usually used for treatment. Resistance rates are increasing dramatically over time.
Even common outpatient infections are becoming resistant to the usual antibiotics. Urinary tract infections (UTIs) are one of the most common infections in the United States, with approximately 10.5 million infections treated per year, at a cost of $3 billion. According to the National Institute of Health, antibiotic-resistant UTIs are increasing rapidly. One in three UTIs are resistant to trimethoprim-sulfamethoxazole, which used to be a universal treatment. One in five UTIs are resistant to at least five antibiotics with some UTIs now resistant to all available drugs.
Antibiogram Resistance, MDPI Antibiotics
Green=Susceptible, Yellow=Intermediate, Red=Resistant
The worldwide impact of resistant bacteria is even more staggering. According to a study published in the Lancet, antimicrobial resistance is an urgent global public health threat. Resistant infections are the direct cause of death of at least 1.27 million people and contribute to almost 5 million deaths per year worldwide. The Review on Antimicrobial Resistance, done at the request of the UK Government, predicted that infections caused by antibiotic-resistant bacteria could kill 10 million people annually by the year 2050.
Antimicrobial Resistance Collaborators, The Lancet
What causes antibiotic resistance?
It's winter now, and there are lots of illnesses going around. Many of them are viral upper respiratory infections. Unfortunately, there is a tendency for people to take antibiotics for viral illnesses. Antibiotics don't kill viruses. Not only do antibiotics not cure viruses, but they can cause significant harm. They can kill off good, healthy bacteria, and make room for harmful bacteria to move in and cause infections like Claustridium difficile, a severe diarrheal illness. They can also kill off other susceptible bacteria, leaving behind only the bacteria that have tools that enable them to survive the antibiotics. These bacteria reproduce and increase their populations, creating more bacteria that can survive common antibiotics. The resistant bacteria can also pass a piece of themselves to unrelated bacteria, enabling those bacteria to survive antibiotics. The resistant bacteria can be passed from one person to another, spreading infections that don't respond to the usual antibiotics. Even when antibiotics are used for bacterial infections, they are often too strong and not specific enough for the infection they are intended to treat. This has the same effect of creating resistant bacteria.
In a similar way, unnecessary antibiotic use on farms can also contributes to antimicrobial resistance. Common food germs like E. Coli and Salmonella become resistant when farms or ranches use antibiotics inappropriately, usually as an attempt to promote animal growth rather than to treat infections. These resistant infections can spread to humans when we consume contaminated food. To combat the issue, farms should only use antibiotics with veterinary oversight to manage and treat infections, not to promote growth.
Alamy
What strategies do germs use to evade antibiotics?
Germs develop new ways of functioning that eliminate the activities that used to be disrupted by antibiotics
Germs use enzymes or proteins that destroy the antibiotics
Germs create barriers that prevent antibiotics from reaching them
Germs change the antibiotics' attachment points (targets) so the antibiotics no longer connect to the germs to affect them
Germs use pumps to eliminate antibiotics from inside them
One resistant germ can spread these strategies to surrounding germs that may not initially have been resistant to antibiotics
Which antibiotic resistant infections are the most severe?
The National Institute of Health has provided the following information on the six most concerning antimicrobial-resistant infections in the United States:
Mycobacterium tuberculosis
The bacteria that causes tuberculosis (TB) is airborne and can cause severe disease. TB most commonly affects the lungs, but may affect many other organs. It must be treated with a regimen of several drugs taken for six months to two years, depending on the type of infection. In most cases, TB is treatable. However, some multi-drug resistant bacteria are becoming resistant to the two most potent TB drugs.
Tuberculosis Lung Infection,Wikipedia
C. difficile
Claustridium difficile is a germ that can infect the colon following antibiotic treatment. The good bacteria that normally live in the gut can help prevent C. difficile colonization and disease. Antibiotic treatment can kill the good bacteria and allow C. difficile, which is naturally resistant to many common antibiotics, to grow and cause inflammation in the colon. C. difficile is a major health care-associated infection in the U.S., causing mild to severe diarrhea. Around half a million people are infected each year, resulting in approximately 15,000 deaths.
VRE
Vancomycin-resistant Enterococci are bacteria that commonly colonize the human digestive tract and female genital tract. VRE infections tend to occur in people who are in hospitals or other health care facilities. They also occur in people who are susceptible to infection because of other medical problems or who have catheters or other medical devices. Health care providers commonly use the antibiotic vancomycin to treat Enterococcal infections, but VRE are resistant to this antibiotic.
MRSA
During the past four decades, methicillin-resistant Staphylococcus aureus, (MRSA) has evolved from a controllable nuisance into a serious public health concern. MRSA is one of the most common hospital-acquired infections. Increasingly, strains are circulating in the community and can cause severe infections. These skin infections can spread rapidly after natural disasters.
MRSA, Dermatology Care of Charlotte
Neisseria gonorrhoea
Gonorrhea is a sexually transmitted infection and the second most commonly reported infection in the U.S. Untreated infections can cause severe reproductive complications, most commonly affecting sexual, racial, and ethnic minorities. Gonorrhea control relies on rapid identification and treatment of infected people and their sexual partners. Some drugs are becoming less effective in treating gonorrhea, and shots of antibiotics are commonly required for treatment. These antibiotic shots are sometimes difficult to find, as they are frequently on back-order.
CRE
Carbapenem-resistant Enterobacteriaceae is a family of highly resistant bacteria that includes Klebsiella species and Escherichia coli. CRE primarily affect patients in hospitals and those who have compromised immune systems. The bacteria can enter the body through medical devices like ventilators or catheters. Some CRE infections are resistant to most available antibiotics and can be life-threatening.
Who is most susceptible to resistant infections?
Children
Elderly
Immunosuppressed patients
Patients taking medications that lower the function of the immune system
Women (with regards to urinary tract infections)
People with diabetes
People with multiple sexual partners
People living in crowded conditions in which infections spread more easily
Patients with cancer
Patients with organ transplants
Patients on dialysis
Patients treated with antibiotics
Hospitalized patients
Richmar
How can antibiotics and antimicrobial resistance affect me?
Antimicrobial resistance makes it harder to treat infections. Medications that used to commonly treat infections no longer work. Instead of taking a simple antibiotic that is well tolerated and has less side effects, it may be necessary to take a more powerful antibiotic that has more side effects and is less tolerable. Higher doses may be required for longer periods of time. Due to antibiotic failure, infections can get worse, such as urine infections progressing to kidney infections, sepsis (blood infections) and death. In some cases, shots of antibiotics or IV antibiotics may be necessary, which require multiple trips to clinics or hospitals, and cost more money. Some infections can no longer be treated with existing antibiotics, and patients must live with ongoing symptoms and illness. Antimicrobial resistance can also affect other types of infections, such as yeast infections, which are becoming increasingly resistant to diflucan-- a simple, single dose treatment that no longer universally treats yeast.
When antibiotics kill too many good bacteria, there are gaps in the usual population of healthy bacteria that provides protection. When there are not enough good bacteria, it is easy for harmful, opportunistic bacteria to move in and cause infections. This may include yeast infections, which are no longer easy to treat because of diflucan resistance. They may also include severe infections such as Claustridium difficile, which can hospitalize young healthy people with severe diarrhea and dehydration. Killing off too many of the good bacteria in your gut may also cause problems with digestion.
Multiple studies indicate that any antibiotic use can contribute to a higher rate of colon cancer, at an earlier age. More frequent and varied antibiotic treatments are associated with a higher rate of colon cancer. As antibiotic use increases, the risk of colon cancer also becomes higher. This may explain why we are seeing an increase in colon cancer diagnoses in young people in their 30s and 40s, which was previously quite unusual.
How are bacterial infections diagnosed?
Bacterial infections are generally diagnosed by health care professionals. Some are diagnosed by a history and physical examination. llnesses (especially upper respiratory infections) that have lasted for a relatively short period of time are more likely to be caused by viruses. There are some exceptions, such as strep throat, urine infections and skin infections, which can develop over the course of a few days. Some infections have a very typical appearance, such as MRSA skin infections. In some cases, office-based tests, such as urine dipsticks and rapid strep tests are used to diagnose bacterial infections. Some infections must be definitively confirmed by a culture. Cultures can be done on stool, urine, sputum, pus and other samples. It can take several days to get culture results confirming the infection. It takes a bit longer to determine which antibiotic is most appropriate for a specific infection (sensitivity). The sensitivity results determine whether a bacteria is resistant to particular antibiotics. Although everyone wants to be treated as quickly as possible, it can be worthwhile to wait a few days to get culture results and then start the antibiotic that is most appropriate for a specific infection. This is a better alternative than guessing what antibiotic is most appropriate and choosing an incorrect antibiotic that will not help and may contribute to the problem of antibiotic resistance.
Dr. Diana Holdright
How are antibiotic resistant germs treated?
Shutterstock
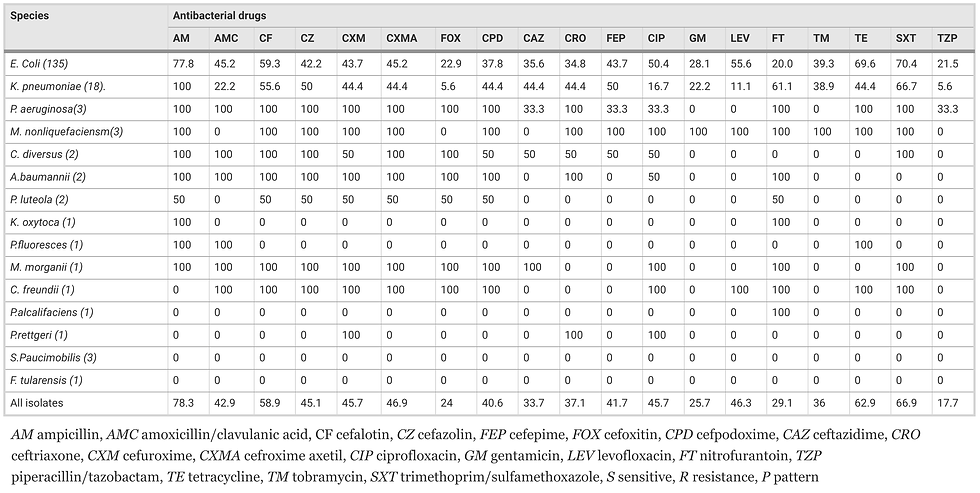
Resistant bacteria may require stronger antibiotics. According to the International Journal of Health Sciences, up to 92% of the bacteria found in urine cultures are resistant to at least one antibiotic. 80% of germs found in urine cultures may be resistant to at least two antibiotics. As antimicrobial resistance increases, there will be fewer antibiotics available to treat bacterial infections. Longer courses of stronger antibiotics may be required to treat bacteria that a decade ago could be treated with a few days of simpler antibiotics. In some cases, IM (shots) or IV (intravenous) antibiotics will be required to treat common bacteria. The choice of antibiotic can be determined by an antibiogram. An antibiogram helps medical professionals know which antibiotics will cover specific germs and infections. Antibiograms may vary tremendously from one part of the country to another, so it is important to know local antibiograms to choose the best antibiotic possible.
Percentage of antibiotic resistance in common urinary tract germs (antibiogram)
BMC Infectious Diseases, Springer Nature
How can I minimize the risks of antibiotic use?
Avoid antibiotics whenever possible! If it is not clear that your infection is bacterial, hold off on antibiotics and monitor closely to see how things change with time and if antibiotics are required. Many infections (even bacterial infections) will improve on their own with time. It is often worthwhile to "wait it out" to see if antibiotics are truly necessary. Make this decision with input from your family physician.
Don't take antibiotics just for the sake of it. If a culture is done and a you are not too unwell, it can be a good idea to wait for culture results so that you are taking the right antibiotic for the infection. This is the best way to make sure your antibiotics are suited to the infection you have. Again, make the decision to await culture results with your doctor.
Most bronchitis and sinus infections are caused by viruses. Antibiotics will not fix them. Green mucus and sputum doesn't mean the infection is bacterial-- it simply means that your immune system (white blood cells) are present and doing their job. If your upper respiratory infection has been going on for less than 10 days, even if you feel like there are symptoms in your airways or your sinuses, a virus is likely the culprit. Antibiotics will NOT fix this! You can improve your symptoms by getting plenty of rest, drinking lots of fluids and humidifying the air around you with a humidifier or steam shower. Over the counter cough and cold medications, and anti-inflammatory medications such as ibuprofen or naproxen can help ease your symptoms while your immune system fights the germs. Warning signs of worsening upper respiratory infections include shortness of breath, chest pain, recurrent or persistent fevers, and bloody sputum.
Just because you felt better with antibiotics doesn't mean that you had a bacterial infection and required antibiotics. Some antibiotics have an anti-inflammatory affect, and taking them is like taking a huge dose of ibuprofen. This will make everyone feel better, and doesn't mean you had a bacterial infection. Save yourself the risk of resistant bacteria and take ibuprofen instead!
Prevent urine infections (UTIs) by hydrating well, and urinating when you have to instead of trying to hold your urine. Urinate after intercourse to "flush out your plumbing", and always wipe from front to back. Some people take supplements such as cranberry capsules or D-mannose to prevent UTIs. Urine tests can help distinguish between UTIs and sexually transmitted infections, and it is worthwhile to get test results to avoid to starting unnecessary antibiotics. Concerning symptoms for worsening infection include back pain, severe abdominal pain, high fevers, nausea and vomiting.
Most cases of diarrhea will improve on their own. Even traveler's diarrhea doesn't always require antibiotics. Stool studies can help determine whether you require antibiotics or not. Antibiotics will commonly cause or worsen diarrhea and can make you feel worse, especially if they are not truly needed to cure your infection. You can help yourself get better faster by drinking plenty of fluids and staying well hydrated. Dairy may be difficult to digest if you have an upset stomach, and you should drink lots of clear liquids, or liquids that you can see through when you hold them up to the light. Liquids like water, broth, jello, sports drinks and watered down juices are good ways to stay hydrated. Bland foods, such as the BRAT (Bananas, Rice, Applesauce, Toast) diet may be easier to digest and help you transition back to a normal diet for a short period while you are recovering. Over the counter anti-diarrheal medications may help you feel better in the short term. Your physician can prescribe an anti-nausea medication if needed. Concerning symptoms include blood or pus in the stools, high fevers, severe abdominal pain and inability to hydrate.
Five things the Center for Disease Control wants you to know about antibiotics:
Antibiotic resistance occurs when germs defeat the drugs designed to kill them. It does NOT mean the body is resistant to antibiotics.
Antibiotic resistance can affect people at any stage of life. Infections caused by resistant germs are difficult—sometimes impossible—to treat. In many cases, these infections require extended hospital stays, additional follow-up doctor visits, and the use of treatments that may be costly and potentially toxic to the patient.
Healthy habits can protect you from infections and help stop germs from spreading. Get recommended vaccines, keep hands and wounds clean, and take good care of chronic conditions, like diabetes.
Antibiotics save human and animal lives. However, any time antibiotics are used, they can lead to side effects and resistance. Antibiotics do not work on viruses, such as colds and the flu. Talk to your healthcare provider or veterinarian about whether antibiotics are needed.
Antibiotic resistance has been found in all regions of the world. Modern trade and travel mean AR can move easily across borders. It can spread in places like hospitals, farms, the community, and the environment. Tell your healthcare provider if you recently traveled to or received care in another country
Does any of this really make a difference? YES!
Center for Disease Control
According to the Center for Disease Control, you should wash your hands with soap and water to prevent infections:
Before, during, and after preparing food
Before eating
Before and after caring for someone at home who is sick with vomiting or diarrhea
Before and after treating a cut or wound
After using the toilet
After changing diapers or cleaning up a child who has used the toilet
After touching an animal, animal feed, or animal waste
After handling pet food or pet treats
After touching garbage
If your hands are visibly dirty or greasy
After blowing your nose, coughing, or sneezing, you should immediately clean your hands by either washing them with soap and water or using hand sanitizer with at least 60% alcohol
Freepik
Which is better for preventing illness-- handwashing or hand sanitizer?
Center for Disease Control
Ember Opinion:
The experts (CDC, Center for Disease Control) recommend washing hands to remove dirt, germs and chemicals. Hand sanitizer is more precise at killing bacteria and most viruses, but doesn't eliminate as many different things as washing with soap and water. Soap and water removes germs that sanitizer might not kill, such as norovirus and Claustridium difficile which can cause bad diarrhea. Soap and water also eliminates other harmful things from the skin, such as contaminated dirt, pesticides and heavy metals. Non-perfumed, non-tar soaps are gentler on the skin. The front and back of hands should be washed for a total of at least 20 seconds to remove as much bacteria as possible. If soap and water is not available, hand sanitizer with at least 60% alcohol can be used as an alternative. I think that hand sanitizer is an easier option, and is more portable, which is an advantage over soap and water. If you can see dirt on your hands, definitely wash with soap and water. But for improving convenience, I prefer hand sanitizer.
Lemelson Center
The Center for Disease Control recommends these steps to minimize the risk from bacteria that is resistant to antibiotics:
Know Your Risks, Ask Questions, & Take Care. Ask your healthcare provider about risks for certain infections and sepsis. Speak up with questions or concerns.
Keep cuts clean and covered until healed, and take good care of chronic conditions, like diabetes or heart disease.
Clean Your Hands Keeping your hands clean is one of the best ways to prevent infections, avoid getting sick, and prevent spreading germs.
Get Vaccinated Vaccines are an important step to prevent infections, including resistant infections.
Be Aware of Changes in Your Health. Talk to your healthcare provider about how to recognize signs and symptoms of infections, or if you think you have an infection. If an infection isn’t stopped, it can lead to additional complications like sepsis, a life-threatening medical emergency.
Use Antibiotics Appropriately. Talk with your healthcare provider or veterinarian about the best treatment when you, your family, or your animal is sick. Antibiotics save lives, but any time they are used they can cause sides effects and lead to antibiotic resistance.
Practice Healthy Habits Around Animals Always clean your hands after touching, feeding, or caring for animals, and keep your animals healthy.
Prepare Food Safely Follow four simple steps to avoid foodborne infections. Clean your hands, cooking utensils, and surfaces. Separate raw meat from other foods. Cook foods to safe temperatures. Chill leftovers and other foods promptly.
Stay Healthy When Traveling Abroad Be vigilant when traveling abroad. Know what vaccinations are needed, check health alerts, stick to safe food and drinks, plan in advance in case you get sick, and learn about the risks of medical tourism.
Prevent STDs Gonorrhea, a common STD, can be resistant to the drugs designed to treat it. The only way to avoid STDs is to not have sex. If you have sex, lower your risk by choosing safer sexual activities and using condoms the right way from start to finish. You and your partner should be treated right away if you test positive to keep from getting infected again.
How can I learn more?























Comments